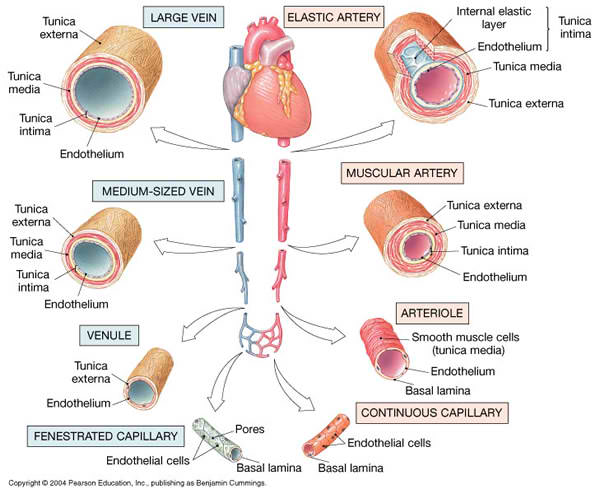
The smallest arterial branches are called arterioles. From the arterioles, blood moves into the capillaries , where diffusion occurs between blood and interstitial fluid. From the capillaries, blood enters small venules, which unite to form larger veins that return blood to the heart. Two major arteries are connected to the heart, one associated with each ventricle.
Several hundred million tiny arterioles provide blood to more than 10 billion capillaries. These capillaries, barely the diameter of a single red blood cell, form extensive, branching networks. If all the capillaries in your body were placed end to end, they would circle the globe with a combined length of over 25,000 miles. The vital functions of the cardiovascular system depend entirely on events at the capillary level: All chemical and gaseous exchange between blood and interstitial fluid takes place across capillary walls.
Several hundred million tiny arterioles provide blood to more than 10 billion capillaries. These capillaries, barely the diameter of a single red blood cell, form extensive, branching networks. If all the capillaries in your body were placed end to end, they would circle the globe with a combined length of over 25,000 miles. The vital functions of the cardiovascular system depend entirely on events at the capillary level: All chemical and gaseous exchange between blood and interstitial fluid takes place across capillary walls.
The Anatomy of Blood Vessels
The pressures experienced by vessels vary with distance from the heart, and their structures reflect this fact. Moreover, arteries, veins, and capillaries differ in function, and these functional differences, as always, involve particular structural adaptations
The pressures experienced by vessels vary with distance from the heart, and their structures reflect this fact. Moreover, arteries, veins, and capillaries differ in function, and these functional differences, as always, involve particular structural adaptations
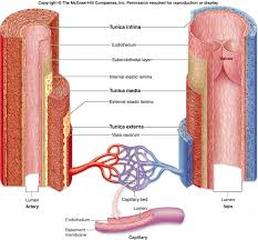
The tunica intima, or tunica interna , is the innermost layer of a blood vessel. In arteries, the outer margin of the tunica intima contains a thick layer of elastic fibers called the internal elastic membrane.
The tunica media , the middle layer, contains concentric sheets of smooth muscle tissue in a framework of loose connective tissue. When these smooth muscles contract, the vessel decreases in diameter; when they relax, the diameter increases.
The tunica externa, or tunica adventitia, is the outermost layer of a blood vessel and forms a connective tissue sheath. The connective–tissue fibers of the tunica externa typically blend into those of adjacent tissues, stabilizing and anchoring the blood vessel.
The walls of large vessels contain small arteries and veins that supply the smooth muscle cells and fibroblasts of the tunica media and tunica externa. These blood vessels are called the vasa vasorum ("vessels of vessels").
The tunica media , the middle layer, contains concentric sheets of smooth muscle tissue in a framework of loose connective tissue. When these smooth muscles contract, the vessel decreases in diameter; when they relax, the diameter increases.
The tunica externa, or tunica adventitia, is the outermost layer of a blood vessel and forms a connective tissue sheath. The connective–tissue fibers of the tunica externa typically blend into those of adjacent tissues, stabilizing and anchoring the blood vessel.
The walls of large vessels contain small arteries and veins that supply the smooth muscle cells and fibroblasts of the tunica media and tunica externa. These blood vessels are called the vasa vasorum ("vessels of vessels").
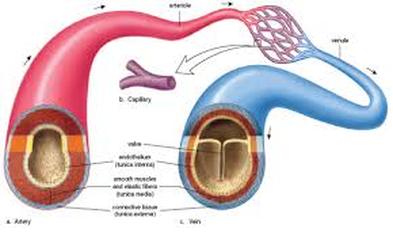
Differences Between Arteries and Veins
Arteries and veins servicing the same region typically lie side by side.
Arteries and veins servicing the same region typically lie side by side.
- In general, the walls of arteries are thicker than those of veins.
- When not opposed by blood pressure, the elastic fibers in the arterial walls recoil, constricting the lumen.
- The endothelial lining of an artery cannot contract, so when an artery constricts, its endothelium is thrown into folds that give arterial sections a pleated appearance. The lining of a vein lacks these folds.
- The thicker walls of the arteries can be felt if the vessels are compressed.
- Arteries usually retain their cylindrical shape, whereas veins often collapse.
- Arteries are more resilient: When stretched, they keep their shape and elongate, and when released, they snap back. A small vein cannot tolerate as much distortion without collapsing or tearing.
- Veins typically contain valves –internal structures that prevent the backflow of blood toward the capillaries
Arteries
When stimulated, arterial smooth muscles contract and thereby constrict the artery–a process called vasoconstriction. Relaxation of these smooth muscles increases the diameter of the lumen–a process called vasodilation . Vasoconstriction and vasodilation affect (1) the afterload on the heart, (2) peripheral blood pressure, and (3) capillary blood flow.
Elastic arteries , or conducting arteries , are large vessels with a diameter up to 2.5 cm (1 in.). These vessels transport large volumes of blood away from the heart. The pulmonary trunk and aorta, as well as their major arterial branches (the pulmonary, common carotid, subclavian , and common iliac arteries ), are elastic arteries.
Muscular arteries , also known as medium–sized arteries or distribution arteries , distribute blood to the body's skeletal muscle and internal organs. Most of the vessels of the arterial system are muscular arteries. The external carotid arteries of the neck, the brachial arteries of the arms, the mesenteric arteries of the abdomen, and the femoral arteries of the thighs are examples of muscular arteries.
Arterioles
Arterioles are considerably smaller than muscular arteries. The tunica media of the smallest arterioles contains scattered smooth muscle cells that do not form a complete layer.
When stimulated, arterial smooth muscles contract and thereby constrict the artery–a process called vasoconstriction. Relaxation of these smooth muscles increases the diameter of the lumen–a process called vasodilation . Vasoconstriction and vasodilation affect (1) the afterload on the heart, (2) peripheral blood pressure, and (3) capillary blood flow.
Elastic arteries , or conducting arteries , are large vessels with a diameter up to 2.5 cm (1 in.). These vessels transport large volumes of blood away from the heart. The pulmonary trunk and aorta, as well as their major arterial branches (the pulmonary, common carotid, subclavian , and common iliac arteries ), are elastic arteries.
Muscular arteries , also known as medium–sized arteries or distribution arteries , distribute blood to the body's skeletal muscle and internal organs. Most of the vessels of the arterial system are muscular arteries. The external carotid arteries of the neck, the brachial arteries of the arms, the mesenteric arteries of the abdomen, and the femoral arteries of the thighs are examples of muscular arteries.
Arterioles
Arterioles are considerably smaller than muscular arteries. The tunica media of the smallest arterioles contains scattered smooth muscle cells that do not form a complete layer.
Capillaries
Capillaries are the only blood vessels whose walls permit exchange between the blood and the surrounding interstitial fluids.
Because capillary walls are thin, the diffusion distances are small, so exchange can occur quickly. In addition, blood flows through capillaries relatively slowly, allowing sufficient time for the diffusion or active transport of materials across the capillary walls.
The average diameter of a capillary is very close to that of a single red blood cell. There are two major types of capillaries: (1) continuous capillaries and (2) fenestrated capillaries .
Capillary Structure
(a) A continuous capillary, showing routes for the diffusion of water and solutes. (b) A fenestrated capillary, showing the pores that facilitate diffusion across the endothelial lining.
In a small continuous capillary, a single endothelial cell may wrap all the way around the lumen, just as your hand wraps around a small glass.
Continuous capillaries are located in all tissues except epithelia and cartilage. Continuous capillaries permit the diffusion of water, small solutes, and lipid–soluble materials into the surrounding interstitial fluid, but prevent the loss of blood cells and plasma proteins.
The endothelial cells in specialized continuous capillaries throughout most of the central nervous system and in the thymus are bound together by tight junctions. These capillaries have very restricted permeability characteristics. We discussed one example, the capillaries responsible for the blood–brain barrier.
Fenestrated Capillaries are capillaries that contain "windows," or pores, that span the endothelial lining . The pores permit the rapid exchange of water and solutes as large as small peptides between plasma and interstitial fluid. Examples of fenestrated capillaries include the choroid plexus of the brain and the blood vessels in a variety of endocrine organs, such as the hypothalamus and the pituitary, pineal, and thyroid glands.
Capillary Beds
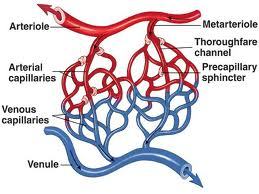
Capillaries do not function as individual units but as part of an interconnected network called a capillary bed , or capillary plexus
A single arteriole generally gives rise to dozens of capillaries that empty into several venules , the smallest vessels of the venous system. The entrance to each capillary is guarded by a band of smooth muscle called a precapillary sphincter . Contraction of the smooth muscle cells constricts and narrows the diameter of the capillary entrance, thereby reducing the flow of blood. Relaxation of the sphincter dilates the opening, allowing blood to enter the capillary faster.
The capillary bed contains several relatively direct connections between arterioles and venules. The wall in the initial part of such a passageway possesses smooth muscles capable of changing its diameter. This segment is called a metarteriole.
A capillary bed may receive blood from more than one artery. The multiple arteries, called collaterals , enter the region and fuse before giving rise to arterioles. The fusion of two collateral arteries that supply a capillary bed is an example of an arterial anastomosis . The interconnections between the anterior and posterior interventricular arteries of the heart are arterial anastomoses
Capillaries are the only blood vessels whose walls permit exchange between the blood and the surrounding interstitial fluids.
Because capillary walls are thin, the diffusion distances are small, so exchange can occur quickly. In addition, blood flows through capillaries relatively slowly, allowing sufficient time for the diffusion or active transport of materials across the capillary walls.
The average diameter of a capillary is very close to that of a single red blood cell. There are two major types of capillaries: (1) continuous capillaries and (2) fenestrated capillaries .
Capillary Structure
(a) A continuous capillary, showing routes for the diffusion of water and solutes. (b) A fenestrated capillary, showing the pores that facilitate diffusion across the endothelial lining.
In a small continuous capillary, a single endothelial cell may wrap all the way around the lumen, just as your hand wraps around a small glass.
Continuous capillaries are located in all tissues except epithelia and cartilage. Continuous capillaries permit the diffusion of water, small solutes, and lipid–soluble materials into the surrounding interstitial fluid, but prevent the loss of blood cells and plasma proteins.
The endothelial cells in specialized continuous capillaries throughout most of the central nervous system and in the thymus are bound together by tight junctions. These capillaries have very restricted permeability characteristics. We discussed one example, the capillaries responsible for the blood–brain barrier.
Fenestrated Capillaries are capillaries that contain "windows," or pores, that span the endothelial lining . The pores permit the rapid exchange of water and solutes as large as small peptides between plasma and interstitial fluid. Examples of fenestrated capillaries include the choroid plexus of the brain and the blood vessels in a variety of endocrine organs, such as the hypothalamus and the pituitary, pineal, and thyroid glands.
Capillary Beds
Capillaries do not function as individual units but as part of an interconnected network called a capillary bed , or capillary plexus
A single arteriole generally gives rise to dozens of capillaries that empty into several venules , the smallest vessels of the venous system. The entrance to each capillary is guarded by a band of smooth muscle called a precapillary sphincter . Contraction of the smooth muscle cells constricts and narrows the diameter of the capillary entrance, thereby reducing the flow of blood. Relaxation of the sphincter dilates the opening, allowing blood to enter the capillary faster.
The capillary bed contains several relatively direct connections between arterioles and venules. The wall in the initial part of such a passageway possesses smooth muscles capable of changing its diameter. This segment is called a metarteriole.
A capillary bed may receive blood from more than one artery. The multiple arteries, called collaterals , enter the region and fuse before giving rise to arterioles. The fusion of two collateral arteries that supply a capillary bed is an example of an arterial anastomosis . The interconnections between the anterior and posterior interventricular arteries of the heart are arterial anastomoses
Veins
Venous walls need not be as thick as arterial walls because the blood pressure in veins is lower than that in the arteries. Veins are classified on the basis of their size. Even though their walls are thinner, veins are in general, larger in diameter than their corresponding arteries.
Venules, which collect blood from capillary beds, are the smallest venous vessels. They vary widely in size and character.
Medium–sized veins range from 2 to 9 mm in internal diameter, comparable in size to muscular arteries. In these veins, the tunica media is thin and contains relatively few smooth muscle cells. The thickest layer of a medium–sized vein is the tunica externa, which contains longitudinal bundles of elastic and collagen fibers.
Large veins include the superior and inferior venae cavae and their tributaries within the abdominopelvic and thoracic cavities. All the tunica layers are present in large veins.
Venous walls need not be as thick as arterial walls because the blood pressure in veins is lower than that in the arteries. Veins are classified on the basis of their size. Even though their walls are thinner, veins are in general, larger in diameter than their corresponding arteries.
Venules, which collect blood from capillary beds, are the smallest venous vessels. They vary widely in size and character.
Medium–sized veins range from 2 to 9 mm in internal diameter, comparable in size to muscular arteries. In these veins, the tunica media is thin and contains relatively few smooth muscle cells. The thickest layer of a medium–sized vein is the tunica externa, which contains longitudinal bundles of elastic and collagen fibers.
Large veins include the superior and inferior venae cavae and their tributaries within the abdominopelvic and thoracic cavities. All the tunica layers are present in large veins.
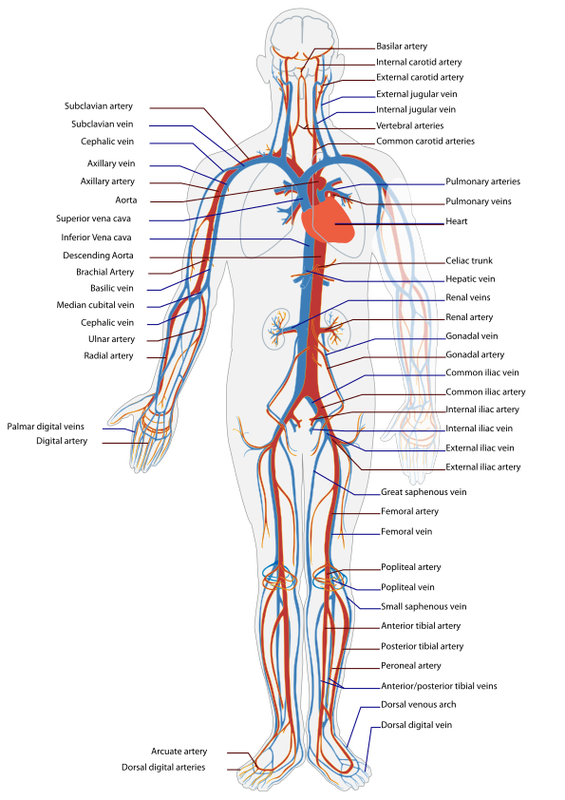
The Circulation of Blood
The human circulatory system is really a two-part system whose purpose is to bring oxygen-bearing blood to all the tissues of the body. When the heart contracts it pushes the blood out into two major loops or cycles. In the systemic loop, the blood circulates into the body’s systems, bringing oxygen to all its organs, structures and tissues and collecting carbon dioxide waste. In the pulmonary loop, the blood circulates to and from the lungs, to release the carbon dioxide and pick up new oxygen. The systemic cycle is controlled by the left side of the heart, the pulmonary cycle by the right side of the heart. Let’s look at what happens during each cycle:
The systemic loop begins when the oxygen-rich blood coming from the lungs enters the upper left chamber of the heart, the left atrium. As the chamber fills, it presses open themitral valve and the blood flows down into the left ventricle. When the ventricles contract during a heartbeat, the blood on the left side is forced into the aorta. This largest artery of the body is an inch wide. The blood leaving the aorta brings oxygen to all the body’s cells through the network of ever smaller arteries and capillaries. The used blood from the body returns to the heart through the network of veins. All of the blood from the body is eventually collected into the two largest veins: the superior vena cava, which receives blood from the upper body, and the inferior vena cava, which receives blood from the lower body region. Both venae cavae empty the blood into the right atrium of the heart.
From here the blood begins its journey through the pulmonary cycle. From the right atrium the blood descends into the right ventricle through the tricuspid valve. When the ventricle contracts, the blood is pushed into the pulmonary artery that branches into two main parts: one going to the left lung, one to the right lung. The fresh, oxygen-rich blood returns to the left atrium of the heart through the pulmonary veins.
Although the circulatory system is made up of two cycles, both happen at the same time. The contraction of the heart muscle starts in the two atria, which push the blood into the ventricles. Then the walls of the ventricles squeeze together and force the blood out into the arteries: the aorta to the body and the pulmonary artery to the lungs. Afterwards, the heart muscle relaxes, allowing blood to flow in from the veins and fill the atria again. In healthy people the normal (resting) heart rate is about 72 beats per minute, but it can go much higher during strenuous exercise. Scientists have estimated that it takes about 30 seconds for a given portion of the blood to complete the entire cycle: from lungs to heart to body, back to the heart and out to the lungs.
The human circulatory system is really a two-part system whose purpose is to bring oxygen-bearing blood to all the tissues of the body. When the heart contracts it pushes the blood out into two major loops or cycles. In the systemic loop, the blood circulates into the body’s systems, bringing oxygen to all its organs, structures and tissues and collecting carbon dioxide waste. In the pulmonary loop, the blood circulates to and from the lungs, to release the carbon dioxide and pick up new oxygen. The systemic cycle is controlled by the left side of the heart, the pulmonary cycle by the right side of the heart. Let’s look at what happens during each cycle:
The systemic loop begins when the oxygen-rich blood coming from the lungs enters the upper left chamber of the heart, the left atrium. As the chamber fills, it presses open themitral valve and the blood flows down into the left ventricle. When the ventricles contract during a heartbeat, the blood on the left side is forced into the aorta. This largest artery of the body is an inch wide. The blood leaving the aorta brings oxygen to all the body’s cells through the network of ever smaller arteries and capillaries. The used blood from the body returns to the heart through the network of veins. All of the blood from the body is eventually collected into the two largest veins: the superior vena cava, which receives blood from the upper body, and the inferior vena cava, which receives blood from the lower body region. Both venae cavae empty the blood into the right atrium of the heart.
From here the blood begins its journey through the pulmonary cycle. From the right atrium the blood descends into the right ventricle through the tricuspid valve. When the ventricle contracts, the blood is pushed into the pulmonary artery that branches into two main parts: one going to the left lung, one to the right lung. The fresh, oxygen-rich blood returns to the left atrium of the heart through the pulmonary veins.
Although the circulatory system is made up of two cycles, both happen at the same time. The contraction of the heart muscle starts in the two atria, which push the blood into the ventricles. Then the walls of the ventricles squeeze together and force the blood out into the arteries: the aorta to the body and the pulmonary artery to the lungs. Afterwards, the heart muscle relaxes, allowing blood to flow in from the veins and fill the atria again. In healthy people the normal (resting) heart rate is about 72 beats per minute, but it can go much higher during strenuous exercise. Scientists have estimated that it takes about 30 seconds for a given portion of the blood to complete the entire cycle: from lungs to heart to body, back to the heart and out to the lungs.
Credits to the owner: http://www.as.miami.edu/chemistry/2086/Chapter_21/NEW-Chap21_class_part1.htm
Credits to the owner: http://lsa.colorado.edu/essence/texts/heart.html
Credits to the owner: http://lsa.colorado.edu/essence/texts/heart.html