Blood is the fluid of life, transporting oxygen from the lungs to body tissue and carbon dioxide from body tissue to the lungs. Blood is the fluid of growth, transporting nourishment from digestion and hormones from glands throughout the body. Blood is the fluid of health, transporting disease fighting substances to the tissue and waste to the kidneys. Because it contains living cells, blood is alive. Red blood cells and white blood cells are responsible for nourishing and cleansing the body.
Without blood, the human body would stop working.
Without blood, the human body would stop working.
Composition of Blood
Blood is classified as a connective tissue and consists of two main components:
Formed elements are:
Blood is classified as a connective tissue and consists of two main components:
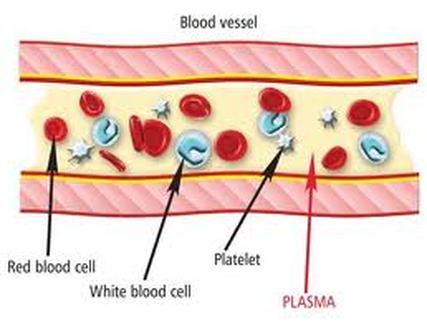
- Plasma, which is a clear extracellular fluid
- Formed elements, which are made up of the blood cells and platelets
Formed elements are:
- Erythrocytes, also known as red blood cells (RBCs)
- Leukocytes, also known as white blood cells (WBCs)
- Platelets
Blood plasma
Blood plasma is a mixture of proteins, enzymes, nutrients, wastes, hormones and gases. The specific composition and function of its components are as follows:
2. Amino acids
These are formed from the break down of tissue proteins or from the digestion of digested proteins.
3. Nitrogenous waste
Being toxic end products of the break down of substances in the body, these are usually cleared from the bloodstream and are excreted by the kidneys at a rate that balances their production.
4. Nutrients
Those absorbed by the digestive tract are transported in the blood plasma. These include glucose, amino acids, fats, cholesterol, phospholipids, vitamins and minerals.
5. Gases
Some oxygen and carbon dioxide are transported by plasma. Plasma also contains a substantial amount of dissolved nitrogen.
6. Electrolytes
The most abundant of these are sodium ions, which account for more of the blood’s osmolarity than any other solute.
Blood plasma is a mixture of proteins, enzymes, nutrients, wastes, hormones and gases. The specific composition and function of its components are as follows:
- Proteins
- They are an important reserve supply of amino acids for cell nutrition. Cells called macrophages in the liver, gut, spleen, lungs and lymphatic tissue can break down plasma proteins so as to release their amino acids. These amino acids are used by other cells to synthesise new products.
- Plasma proteins also serve as carriers for other molecules. Many types of small molecules bind to specific plasma proteins and are transported from the organs that absorb these proteins to other tissues for utilisation. The proteins also help to keep the blood slightly basic at a stable pH. They do this by functioning as weak bases themselves to bind excess H+ ions. By doing so, they remove excess H+ from the blood which keeps it slightly basic.
- The plasma proteins interact in specific ways to cause the blood to coagulate, which is part of the body’s response to injury to the blood vessels (also known as vascular injury), and helps protect against the loss of blood and invasion by foreign microorganisms and viruses.
- Plasma proteins govern the distribution of water between the blood and tissue fluid by producing what is known as a colloid osmotic pressure.
- Albumins, which are the smallest and most abundant plasma proteins. Reductions in plasma albumin content can result in a loss of fluid from the blood and a gain of fluid in the interstitial space (space within the tissue), which may occur in nutritional, liver and kidney disease. Albumin also helps many substances dissolve in the plasma by binding to them, hence playing an important role in plasma transport of substances such as drugs, hormones and fatty acids.
- Globulins, which can be subdivided into three classes from smallest to largest in molecular weight into alpha, beta and gamma globulins. The globulins include high density lipoproteins (HDL), an alpha-1 globulin, and low density lipoproteins (LDL), a beta-1 globulin. HDL functions in lipid transport carrying fats to cells for use in energy metabolism, membrane reconstruction and hormone function. HDLs also appear to prevent cholesterol from invading and settling in the walls of arteries. LDL carries cholesterol and fats to tissues for use in manufacturing steroid hormones and building cell membranes, but it also favours the deposition of cholesterol in arterial walls and thus appears to play a role in disease of the blood vessels and heart. HDL and LDL therefore play important parts in the regulation of cholesterol and hence have a large impact on cardiovascular disease.
- Fibrinogen, which is a soluble precursor of a sticky protein called fibrin, which forms the framework of blood clot. Fibrin plays a key role in coagulation of blood, which is discussed later in this article under Platelets.
2. Amino acids
These are formed from the break down of tissue proteins or from the digestion of digested proteins.
3. Nitrogenous waste
Being toxic end products of the break down of substances in the body, these are usually cleared from the bloodstream and are excreted by the kidneys at a rate that balances their production.
4. Nutrients
Those absorbed by the digestive tract are transported in the blood plasma. These include glucose, amino acids, fats, cholesterol, phospholipids, vitamins and minerals.
5. Gases
Some oxygen and carbon dioxide are transported by plasma. Plasma also contains a substantial amount of dissolved nitrogen.
6. Electrolytes
The most abundant of these are sodium ions, which account for more of the blood’s osmolarity than any other solute.
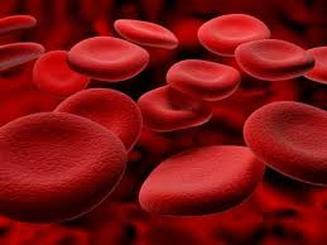
Red blood cells
Red blood cells (RBCs), also known as erythrocytes, have two main functions:
RBCs are incapable of aerobic respiration, preventing them from consuming the oxygen they transport because they lose nearly all their inner cellular components during maturation. The inner cellular components lost include their mitochondria, which normally provide energy to a cell, and their nucleus, which contains the genetic material of the cell and enable it to repair itself. The lack of a nucleus means that RBCs are unable to repair themselves. However, the resulting biconcave shape is that the cell has a greater ratio of surface area to volume, enabling O2 and CO2 to diffuse quickly to and from Hb.
The cytoplasm of a RBC consists mainly of a 33% solution of haemoglobin (Hb), which gives RBCs their red colour. Haemoglobin carries most of the oxygen and some of the carbon dioxide transported by the blood.
Circulating erythrocytes live for about 120 days. As a RBC ages, its membrane grows increasingly fragile. Without key organelles such as a nucleus or ribosomes, RBCs cannot repair themselves. Many RBCs die in the spleen, where they become trapped in narrow channels, broken up and destroyed. Haemolysis refers to the rupture of RBCs, where haemoglobin is released leaving empty plasma membranes which are easily digested by cells known as macrophages in the liver and spleen. The Hb is then further broken down into its different components and either recycled in the body for further use or disposed of.
Red blood cells (RBCs), also known as erythrocytes, have two main functions:
- To pick up oxygen from the lungs and deliver it to tissues elsewhere
- To pick up carbon dioxide from other tissues and unload it in the lungs
RBCs are incapable of aerobic respiration, preventing them from consuming the oxygen they transport because they lose nearly all their inner cellular components during maturation. The inner cellular components lost include their mitochondria, which normally provide energy to a cell, and their nucleus, which contains the genetic material of the cell and enable it to repair itself. The lack of a nucleus means that RBCs are unable to repair themselves. However, the resulting biconcave shape is that the cell has a greater ratio of surface area to volume, enabling O2 and CO2 to diffuse quickly to and from Hb.
The cytoplasm of a RBC consists mainly of a 33% solution of haemoglobin (Hb), which gives RBCs their red colour. Haemoglobin carries most of the oxygen and some of the carbon dioxide transported by the blood.
Circulating erythrocytes live for about 120 days. As a RBC ages, its membrane grows increasingly fragile. Without key organelles such as a nucleus or ribosomes, RBCs cannot repair themselves. Many RBCs die in the spleen, where they become trapped in narrow channels, broken up and destroyed. Haemolysis refers to the rupture of RBCs, where haemoglobin is released leaving empty plasma membranes which are easily digested by cells known as macrophages in the liver and spleen. The Hb is then further broken down into its different components and either recycled in the body for further use or disposed of.
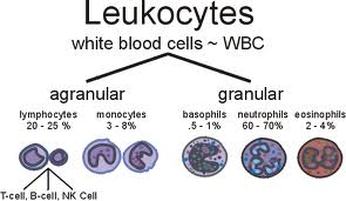
White blood cells
White blood cells (WBCs) are also known as leukocytes. They can be divided into granulocytes and agranulocytes. The former have cytoplasms that contain organelles that appear as coloured granules through light microscopy, hence their name. Granulocytes consist of neutrophils, eosinophils and basophils. In contrast, agranulocytes do not contain granules. They consist of lymphocytes and monocytes.
Granulocytes
Neutrophils: These contain very fine cytoplasmic granules that can be seen under a light microscope. Neutrophils are also called polymorphonuclear (PMN) because they have a variety of nuclear shapes. They play roles in the destruction of bacteria and the release of chemicals that kill or inhibit the growth of bacteria.
Eosinophils: These have large granules and a prominent nucleus that is divided into two lobes. They function in the destruction of allergens and inflammatory chemicals, and release enzymes that disable parasites.
Basophils: They have a pale nucleus that is usually hidden by granules. They secrete histamine which increases tissue blood flow via dilating the blood vessels, and also secrete heparin which is an anticoagulant that promotes mobility of other WBCs by preventing clotting.
Agranulocytes
White blood cells (WBCs) are also known as leukocytes. They can be divided into granulocytes and agranulocytes. The former have cytoplasms that contain organelles that appear as coloured granules through light microscopy, hence their name. Granulocytes consist of neutrophils, eosinophils and basophils. In contrast, agranulocytes do not contain granules. They consist of lymphocytes and monocytes.
Granulocytes
Neutrophils: These contain very fine cytoplasmic granules that can be seen under a light microscope. Neutrophils are also called polymorphonuclear (PMN) because they have a variety of nuclear shapes. They play roles in the destruction of bacteria and the release of chemicals that kill or inhibit the growth of bacteria.
Eosinophils: These have large granules and a prominent nucleus that is divided into two lobes. They function in the destruction of allergens and inflammatory chemicals, and release enzymes that disable parasites.
Basophils: They have a pale nucleus that is usually hidden by granules. They secrete histamine which increases tissue blood flow via dilating the blood vessels, and also secrete heparin which is an anticoagulant that promotes mobility of other WBCs by preventing clotting.
Agranulocytes
- Lymphocytes: These are usually classified as small, medium or large. Medium and large lymphocytes are generally seen mainly in fibrous connective tissue and only occasionally in the circulation bloodstream. Lymphocytes function in destroying cancer cells, cells infected by viruses, and foreign invading cells. In addition, they present antigens to activate other cells of the immune system. They also coordinate the actions of other immune cells, secrete antibodies and serve in immune memory.
- Monocytes: They are the largest of the formed elements. Their cytoplasm tends to be abundant and relatively clear. They function in differentiating into macrophages, which are large phagocytic cells, and digest pathogens, dead neutrophils, and the debris of dead cells. Like lymphocytes, they also present antigens to activate other immune cells.
Platelets
Platelets are small fragments of bone marrow cells and are therefore not really classified as cells themselves.
Platelets have the following functions:
Vascular spasm
This is a prompt constriction of the broken blood vessel and is the most immediate protection against blood loss. Injury stimulates pain receptors. Some of these receptors directly innervate nearby blood vessels and cause them to constrict. After a few minutes, other mechanisms take over. Injury to the smooth muscle of the blood vessel itself causes a longer-lasting vasoconstriction where platelets release a chemical vasoconstrictor called serotonin. This maintains vascular spasm long enough for the other haemostatic mechanisms to come into play.
Platelet plug formation
Under normal conditions, platelets do not usually adhere to the wall of undamaged blood vessels, since the vessel lining tends to be smooth and coated with a platelet repellent. When a vessel is broken, platelets put out long spiny extensions to adhere to the vessel wall as well as to other platelets. These extensions then contract and draw the walls of the vessel together. The mass of platelets formed is known as a platelet plug, and can reduce or stop minor bleeding.
Coagulation
This is the last and most effective defence against bleeding. During bleeding, it is important for the blood to clot quickly to minimise blood loss, but it is equally important for blood not to clot in undamaged vessels. Coagulation is a very complex process aimed at clotting the blood at appropriate amounts. The objective of coagulation is to convert plasma protein fibrinogen into fibrin, which is a sticky protein that adheres to the walls of a vessel. Blood cells and platelets become stuck to fibrin, and the resulting mass helps to seal the break in the blood vessel. The forming of fibrin is what makes coagulation so complicated, as it involved numerous chemicals reactions and many coagulation factors.
Platelets are small fragments of bone marrow cells and are therefore not really classified as cells themselves.
Platelets have the following functions:
- Secrete vasoconstrictors which constrict blood vessels, causing vascular spasms in broken blood vessels
- Form temporary platelet plugs to stop bleeding
- Secrete procoagulants (clotting factors) to promote blood clotting
- Dissolve blood clots when they are no longer needed
- Digest and destroy bacteria
- Secrete chemicals that attract neutrophils and monocytes to sites of inflammation
- Secrete growth factors to maintain the linings of blood vessels
- The first three functions listed above refer to important haemostatic mechanisms in which platelets play a role in during bleeding: vascular spasms, platelet plug formation and blood clotting (coagulation).
Vascular spasm
This is a prompt constriction of the broken blood vessel and is the most immediate protection against blood loss. Injury stimulates pain receptors. Some of these receptors directly innervate nearby blood vessels and cause them to constrict. After a few minutes, other mechanisms take over. Injury to the smooth muscle of the blood vessel itself causes a longer-lasting vasoconstriction where platelets release a chemical vasoconstrictor called serotonin. This maintains vascular spasm long enough for the other haemostatic mechanisms to come into play.
Platelet plug formation
Under normal conditions, platelets do not usually adhere to the wall of undamaged blood vessels, since the vessel lining tends to be smooth and coated with a platelet repellent. When a vessel is broken, platelets put out long spiny extensions to adhere to the vessel wall as well as to other platelets. These extensions then contract and draw the walls of the vessel together. The mass of platelets formed is known as a platelet plug, and can reduce or stop minor bleeding.
Coagulation
This is the last and most effective defence against bleeding. During bleeding, it is important for the blood to clot quickly to minimise blood loss, but it is equally important for blood not to clot in undamaged vessels. Coagulation is a very complex process aimed at clotting the blood at appropriate amounts. The objective of coagulation is to convert plasma protein fibrinogen into fibrin, which is a sticky protein that adheres to the walls of a vessel. Blood cells and platelets become stuck to fibrin, and the resulting mass helps to seal the break in the blood vessel. The forming of fibrin is what makes coagulation so complicated, as it involved numerous chemicals reactions and many coagulation factors.
Circulatory Pathways
The blood vessels of the body are functionally divided into two distinctive circuits: pulmonary circuit and systemic circuit. The pump for the pulmonary circuit, which circulates blood through the lungs, is the right ventricle. The left ventricle is the pump for the systemic circuit, which provides the blood supply for the tissue cells of the body.
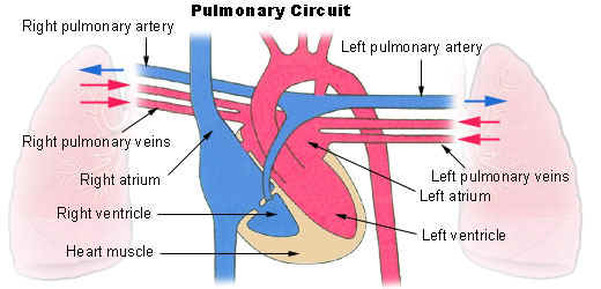
Pulmonary Circuit
Pulmonary circulation transports oxygen-poor blood from the right ventricle to the lungs where blood picks up a new blood supply. Then it returns the oxygen-rich blood to the left atrium.
The blood vessels of the body are functionally divided into two distinctive circuits: pulmonary circuit and systemic circuit. The pump for the pulmonary circuit, which circulates blood through the lungs, is the right ventricle. The left ventricle is the pump for the systemic circuit, which provides the blood supply for the tissue cells of the body.
Pulmonary Circuit
Pulmonary circulation transports oxygen-poor blood from the right ventricle to the lungs where blood picks up a new blood supply. Then it returns the oxygen-rich blood to the left atrium.
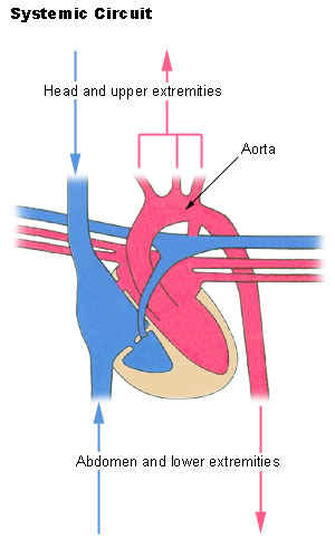
Systemic Circuit
The systemic circulation provides the functional blood supply to all body tissue. It carries oxygen and nutrients to the cells and picks up carbon dioxide and waste products. Systemic circulation carries oxygenated blood from the left ventricle, through the arteries, to the capillaries in the tissues of the body. From the tissue capillaries, the deoxygenated blood returns through a system of veins to the right atrium of the heart.
The coronary arteries are the only vessels that branch from the ascending aorta. The brachiocephalic, left common carotid, and left subclavian arteries branch from the aortic arch. Blood supply for the brain is provided by the internal carotid and vertebral arteries. The subclavian arteries provide the blood supply for the upper extremity. The celiac, superior mesenteric, suprarenal, renal, gonadal, and inferior mesenteric arteries branch from the abdominal aorta to supply the abdominal viscera. Lumbar arteries provide blood for the muscles and spinal cord. Branches of the external iliac artery provide the blood supply for the lower extremity. The internal iliac artery supplies the pelvic viscera.
Major Systemic Arteries
All systemic arteries are branches, either directly or indirectly, from the aorta. The aorta ascends from the left ventricle, curves posteriorly and to the left, then descends through the thorax and abdomen. This geography divides the aorta into three portions: ascending aorta, arotic arch, and descending aorta. The descending aorta is further subdivided into the thoracic arota and abdominal aorta.
Major Systemic Veins
After blood delivers oxygen to the tissues and picks up carbon dioxide, it returns to the heart through a system of veins. The capillaries, where the gaseous exchange occurs, merge into venules and these converge to form larger and larger veins until the blood reaches either the superior vena cava or inferior vena cava, which drain into the right atrium.
Fetal Circulation
Most circulatory pathways in a fetus are like those in the adult but there are some notable differences because the lungs, the gastrointestinal tract, and the kidneys are not functioning before birth. The fetus obtains its oxygen and nutrients from the mother and also depends on maternal circulation to carry away the carbon dioxide and waste products.
The umbilical cord contains two umbilical arteries to carry fetal blood to the placenta and one umbilical vein to carry oxygen-and-nutrient-rich blood from the placenta to the fetus. The ductus venosus allows blood to bypass the immature liver in fetal circulation. The foramen ovale and ductus arteriosus are modifications that permit blood to bypass the lungs in fetal circulation.
The systemic circulation provides the functional blood supply to all body tissue. It carries oxygen and nutrients to the cells and picks up carbon dioxide and waste products. Systemic circulation carries oxygenated blood from the left ventricle, through the arteries, to the capillaries in the tissues of the body. From the tissue capillaries, the deoxygenated blood returns through a system of veins to the right atrium of the heart.
The coronary arteries are the only vessels that branch from the ascending aorta. The brachiocephalic, left common carotid, and left subclavian arteries branch from the aortic arch. Blood supply for the brain is provided by the internal carotid and vertebral arteries. The subclavian arteries provide the blood supply for the upper extremity. The celiac, superior mesenteric, suprarenal, renal, gonadal, and inferior mesenteric arteries branch from the abdominal aorta to supply the abdominal viscera. Lumbar arteries provide blood for the muscles and spinal cord. Branches of the external iliac artery provide the blood supply for the lower extremity. The internal iliac artery supplies the pelvic viscera.
Major Systemic Arteries
All systemic arteries are branches, either directly or indirectly, from the aorta. The aorta ascends from the left ventricle, curves posteriorly and to the left, then descends through the thorax and abdomen. This geography divides the aorta into three portions: ascending aorta, arotic arch, and descending aorta. The descending aorta is further subdivided into the thoracic arota and abdominal aorta.
Major Systemic Veins
After blood delivers oxygen to the tissues and picks up carbon dioxide, it returns to the heart through a system of veins. The capillaries, where the gaseous exchange occurs, merge into venules and these converge to form larger and larger veins until the blood reaches either the superior vena cava or inferior vena cava, which drain into the right atrium.
Fetal Circulation
Most circulatory pathways in a fetus are like those in the adult but there are some notable differences because the lungs, the gastrointestinal tract, and the kidneys are not functioning before birth. The fetus obtains its oxygen and nutrients from the mother and also depends on maternal circulation to carry away the carbon dioxide and waste products.
The umbilical cord contains two umbilical arteries to carry fetal blood to the placenta and one umbilical vein to carry oxygen-and-nutrient-rich blood from the placenta to the fetus. The ductus venosus allows blood to bypass the immature liver in fetal circulation. The foramen ovale and ductus arteriosus are modifications that permit blood to bypass the lungs in fetal circulation.
Credits to the owner: http://www.myvmc.com/anatomy/blood-function-and-composition/